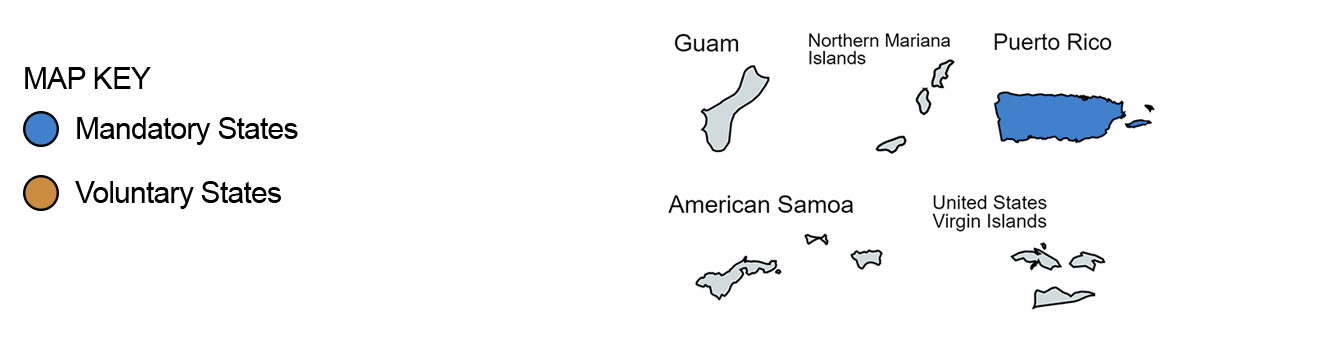
State Disability & Paid Family Leave
LiDAC is one of the leading Distributors of State Disability & Paid Family Leave Services nationally oferring a variety of insured solutions through a host of Insurance Companies. LiDAC has over 40 years of experience in working with brokers and employers to identify, review and address the impact and approach to consider in responding to the evolutionary changes in State Disability and Paid Family Leave on behalf of their employees. LiDAC remains a significant resource prepared to explore, develop and recommend the most beneficial solution for consideration in those states that permit optional insurance coverage through a private carrier state plan.
This informational material is subject to change as we continue to receive guidance from each state. This is not intended and shall not be considered as legal advice. LiDAC assumes no responsibility for compliance related to your business practices, Legal considerations and / or any recommendations as may be contained herein shall not consitute our undertaking on your behalf, or for the benefit of others, to determine or warrant that your business operations are in compliance with any law, rule or regulation. Those seeking resolution of specific legal or business issues, questions, or concerns regarding this topic should consult their own attorney or business advisors.